Featured Services
Photos of both the retina and external eye
“A picture is worth a thousand words” is never as true as it is in ophthalmology. Your eye exam should be able to display baseline photos of your eye condition (disk photos for glaucoma and retinal photos for a choroidal nevus- which is seen in retinal photos) alongside the current photos so you can compare them side by side just like your ophthalmologist does. Changes in either condition are not what we want to see. Here are some examples of disks (abnormal otherwise I wouldn’t be taking photos) and nevuses from my practice. First, side by side optic disk photos comparing different years from the same patient are shown. Each line is a different patient:
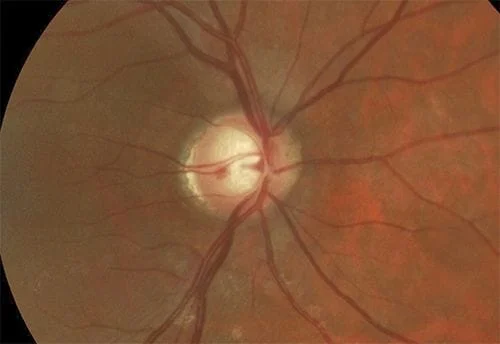
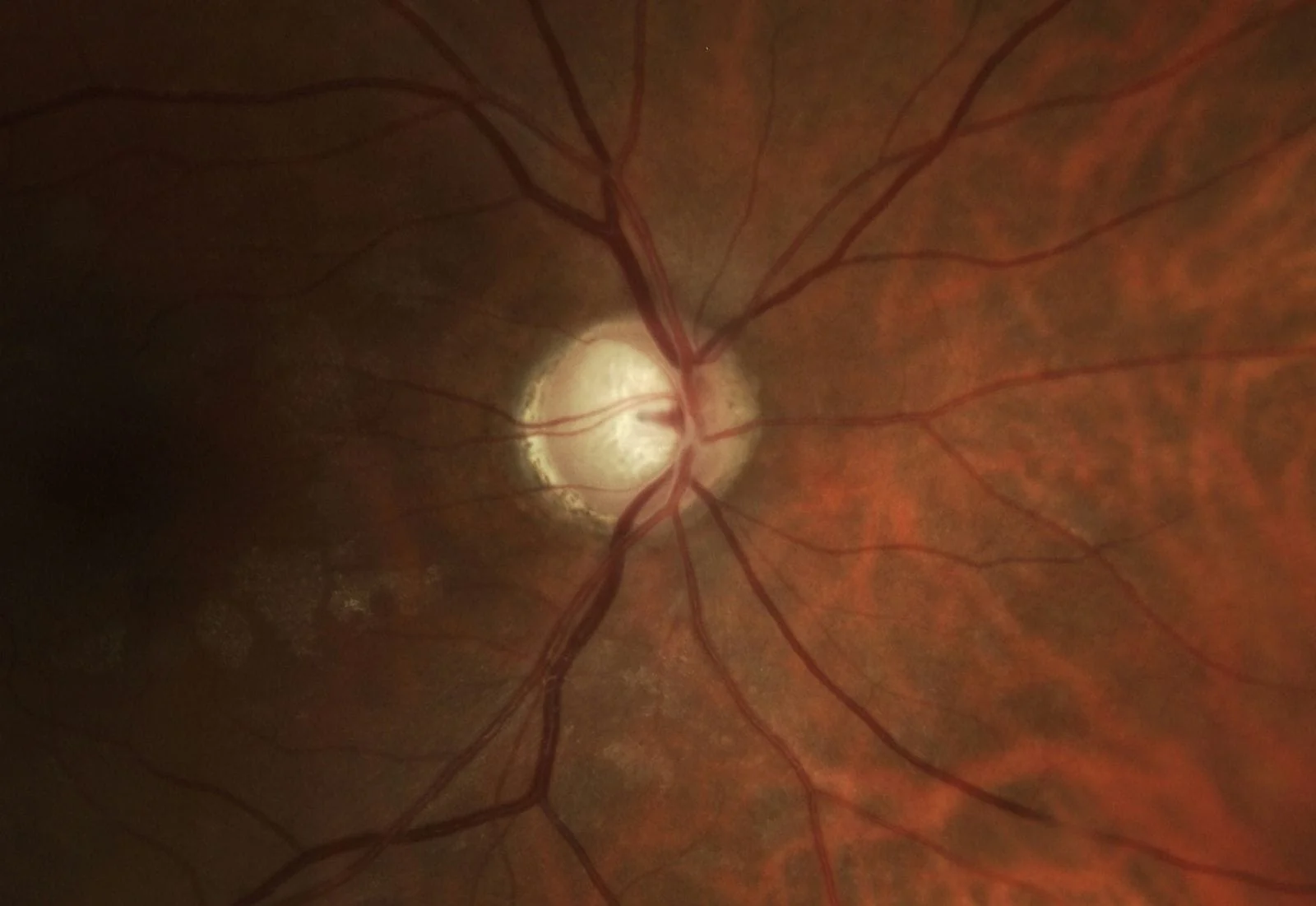
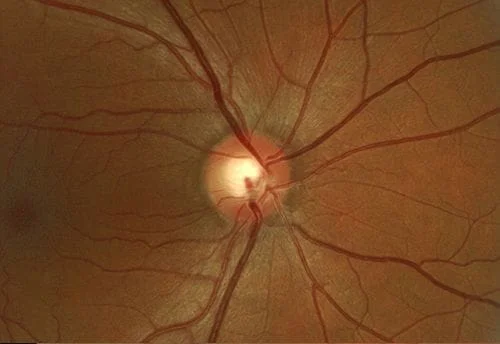
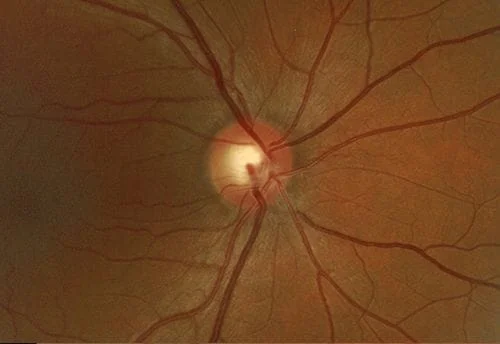
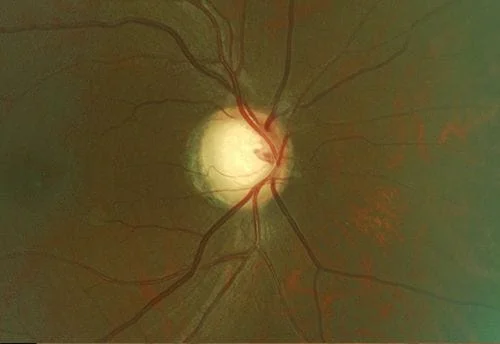
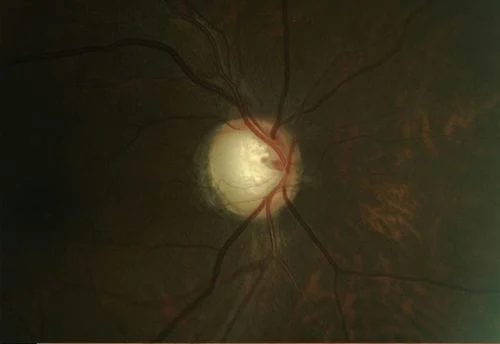
Now some photos of nevuses, again the same patient is shown side by side with 3 different patients shown:
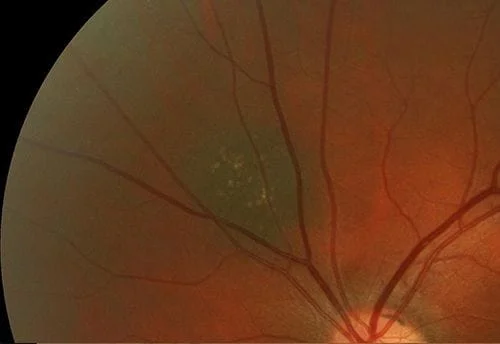
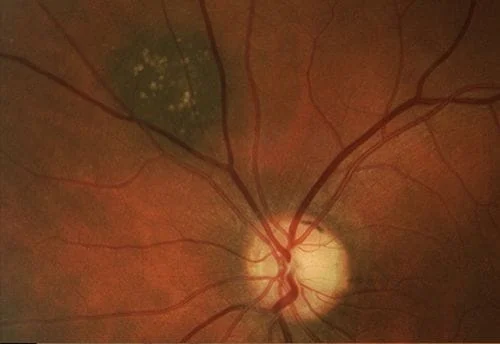
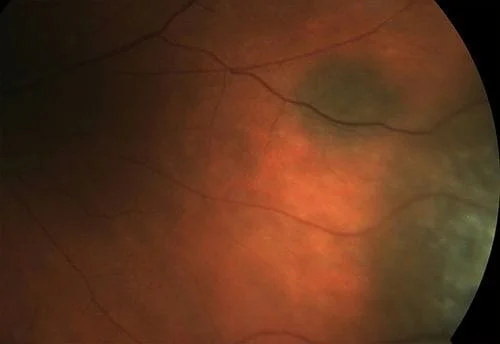
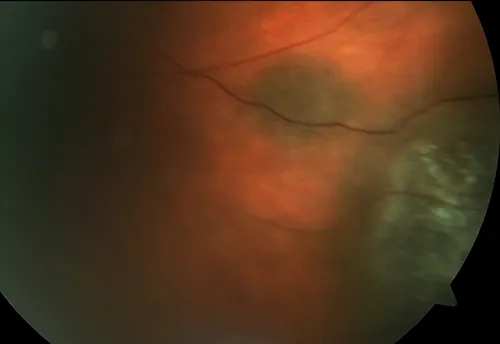
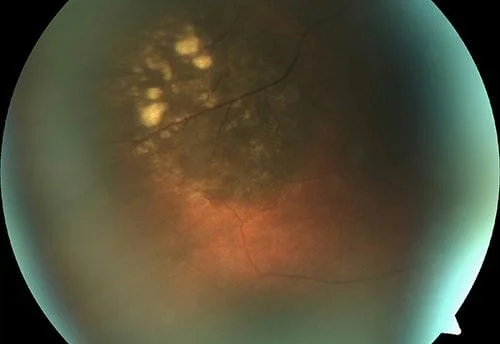
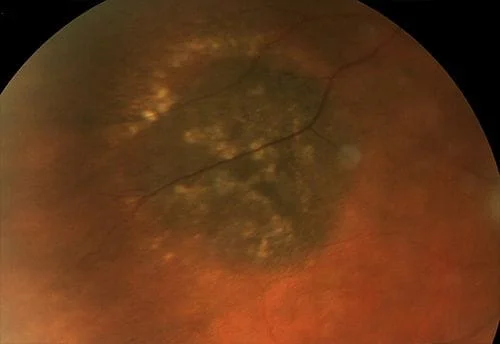
Here are some external photos of the eye. They are called external since they are of conditions on the outside of the eye as opposed to inside the eye as in retinal photos.
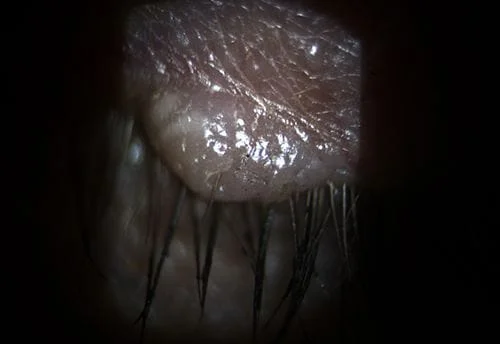
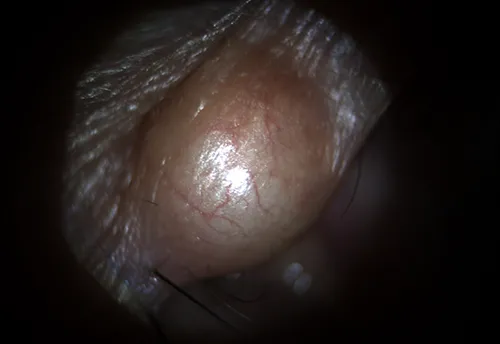
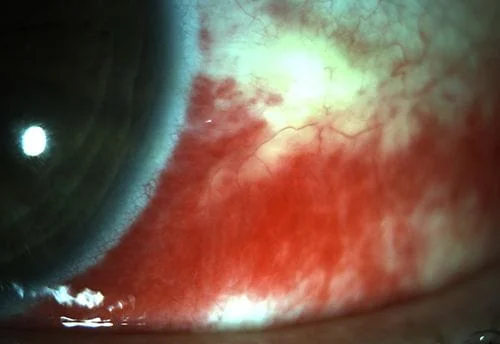
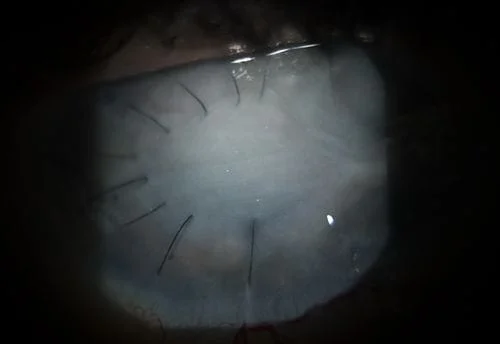
Visual fields
Visual fields test the how well your side vision is. Newer software graphs a progression analysis that is the cutting edge in visual field testing. The middle graph in this read out shows testing done over a number of years (displayed as the patient’s age on the horizontal line) versus the sensitivity of the eye (called the VFI with 100% being normal, shown as the vertical line) all on one graph. Progressive loss has a downward slope as shown in this example. This is not what you want to see as it could mean that someone’s glaucoma damage is getting progressively worse. Rim and other artifacts can make the VFI look like it is getting worse when it isn’t. The machine isn’t smart enough to detect false positive results. Your ophthalmologist is and will tell you if this is the case for your eyes. Your ophthalmologist should have this technology and the read out looks like this:
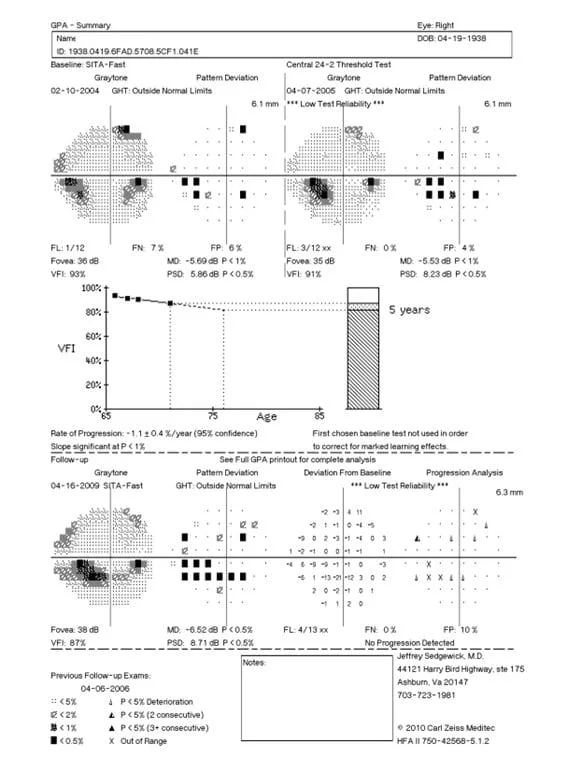
HRT/OCT
Up to 40 to 50% of the optic nerve is dead before the first defect shows up on a visual field test.
(Quigley HA, Dunkelberger GR, et al. Retinal Ganglion Cell Atrophy Correlated with Automated Perimetry in Human Eyes with Glaucoma. Am J Ophthalmology 1989; 107: 453-464 and Quigley HA, Addicks EM, et al. Optic Nerve Damage in Human Glaucoma. Arch Ophthalmology 1982; 100: 135-146).
We have tried for years to reliable detect early glaucoma loss and developed the HRT/ OCT and other machines in order to do just that. An Academy of Ophthalmology paper states that there is no difference between these machines in their sensitivities and specificities when it comes to detecting early glaucoma damage. (Lin SC, Singh K, et al. Optic Nerve Head and Retinal Nerve Fiber Layer Analysis. Ophthalmology 2007; 114: 1937-1949).
Diopsys ERG/VEP
Newer still testing involves the measurement of how well the retina is performing (ERG) and how well the optic nerve is performing (VEP). Newer technology is slowly assimilated in most practices so don’t be too surprised if your ophthalmologists doesn’t have these tests yet.
Gonioscopy and Pachymetry
Both standard tests that should be done at least once on all glaucoma and glaucoma suspect patients.
